Disclaimer :: Dr. Catherine Bevan, a local OB/Gyn, sponsored and created this post based on her expertise.
 Cervical cancer was once a major public health concern in the United States, affecting about 15 in 100,000 women in 1975. In the subsequent 40 years, this rate has more than halved, almost exclusively due to findings made originally in the 1920s by Greek pathologist Georgios Papanikolaou. The Pap (for Papanikolaou) smear is the foundation for one of the great success stories of cancer screening and public health in the United States in general. Many technological advances have been made since the start of widespread screening of reproductive-aged women in the 1970s, but the Pap smear (and its derivations) remains an important component of this process. In this post, I will outline what is involved in cervical cancer screening, how it has changed in recent years, and how it may change in the future.
Cervical cancer was once a major public health concern in the United States, affecting about 15 in 100,000 women in 1975. In the subsequent 40 years, this rate has more than halved, almost exclusively due to findings made originally in the 1920s by Greek pathologist Georgios Papanikolaou. The Pap (for Papanikolaou) smear is the foundation for one of the great success stories of cancer screening and public health in the United States in general. Many technological advances have been made since the start of widespread screening of reproductive-aged women in the 1970s, but the Pap smear (and its derivations) remains an important component of this process. In this post, I will outline what is involved in cervical cancer screening, how it has changed in recent years, and how it may change in the future.
What Is a Pap Smear?
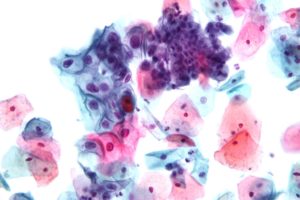
A Pap smear (a.k.a Pap test, cervical smear, smear test) refers to the process of obtaining cells from the cervix and observing them under a microscope to look for changes associated with infection by the Human Papilloma Virus (HPV), the causative agent of cervical cancer. The hope is to catch infection early, before HPV leads to the development of cervical cancer. Dr. Papanikolaou (among others) noticed unique pre-cancerous changes in the cells affected by HPV that can be seen under the microscope. Referring women with these changes for further testing or intervention before the development of cervical cancer has unquestionably saved countless lives. Although components of the Pap smear have changed over the years (for example, the way the sample is collected from the cervix and processed), the basic principle has remained the same. What has changed dramatically are the ancillary tests (namely HPV DNA testing) and the recommended frequency of performing a Pap smear.
 What Is HPV DNA Testing?
What Is HPV DNA Testing?
The Pap smear serves as an indirect test for infection by HPV by looking at cellular changes associated with the virus. HPV DNA testing tests directly for the presence of viral DNA in a sample of cervical cells. DNA testing has allowed for specific detection of high-risk strains of the virus and has served as an invaluable adjunct in cervical cancer screening. The challenge for health care professionals in recent years has been how to incorporate both testing methodologies to maximize the public health benefits while minimizing unnecessary testing and interventions. The recommendations for how often women should be screened for cervical cancer and what tests should be used have changed frequently and are still hotly contested among physicians and public health professionals. Reasonable, competent physicians disagree as to how often women should be screened, and it is important that any concerns you may have regarding testing are voiced to your physician.
What Are the Current Recommendations?
With the caveat that every woman is different, and an individual’s medical history and personal circumstances will supersede general guidelines, here are the current joint recommendations of the major professional organizations involved with cervical cancer screening:
| Population | Recommended Screening Method |
| Women younger than 21 years | No screening |
| Women aged 21-29 years | Pap smear alone every 3 years |
| Women aged 30-65 years | HPV DNA testing and Pap smear every 5 years (preferred)
Pap smear alone every 3 years (acceptable) |
| Women older than 65 years | No screening necessary if negative history |
As you can see, the recommendations have changed drastically from back in the day when it was recommended that every woman get a Pap smear every year at their annual “well woman” exam. Many women wonder whether screening is necessary if they received the HPV vaccine. It is currently recommended that women who have been vaccinated follow the same screening guidelines as everyone else.
While cervical cancer remains a major problem worldwide, cervical cancer screening in the United States has dramatically reduced the risk of obtaining or dying from cervical cancer. As technology continues to develop, the recommendations for cervical cancer screening are likely to continue to change over time. Open communication and discussion with your physician is the best way to stay up to date with regards to these ever-changing guidelines.
 Dr. Catherine Bevan is a board certified obstretician and gynecologist, who practices in Tarrant County, with offices in Fort Worth and Willow Park. She is a Fort Worth native and received her Bachelor of Arts degree from Washington University in St. Louis where she graduated cum laude, Phi Beta Kappa. She then returned to Texas to complete her medical degree at UT Southwestern as well as her residency training at Parkland Memorial Hospital. She also spent an additional year as an assistant professor at UT Southwestern, specializing in gynecologic surgery and emergency women’s care. Providing excellent service to her patients is a passion for her as she guides them to the best possible healthcare outcomes.
Dr. Catherine Bevan is a board certified obstretician and gynecologist, who practices in Tarrant County, with offices in Fort Worth and Willow Park. She is a Fort Worth native and received her Bachelor of Arts degree from Washington University in St. Louis where she graduated cum laude, Phi Beta Kappa. She then returned to Texas to complete her medical degree at UT Southwestern as well as her residency training at Parkland Memorial Hospital. She also spent an additional year as an assistant professor at UT Southwestern, specializing in gynecologic surgery and emergency women’s care. Providing excellent service to her patients is a passion for her as she guides them to the best possible healthcare outcomes.
You can read more from Dr. Bevan on the Fort Worth Moms Blog archives.
Please visit her websites for more information: www.healthcareoftexas.com and www.txhealthcare.com.
You can contact Dr. Bevan at:
- 1250 8th Avenue, Ste 320 // Fort Worth, TX 76104 // (P) 817-924-2111 // (F) 817-564-3980
- 134 El Chico Trail, Suite 103 // Willow Park, TX 76087 // (P) 817-441-1644 // (F) 817-441-1626













